Summary of Key Points:
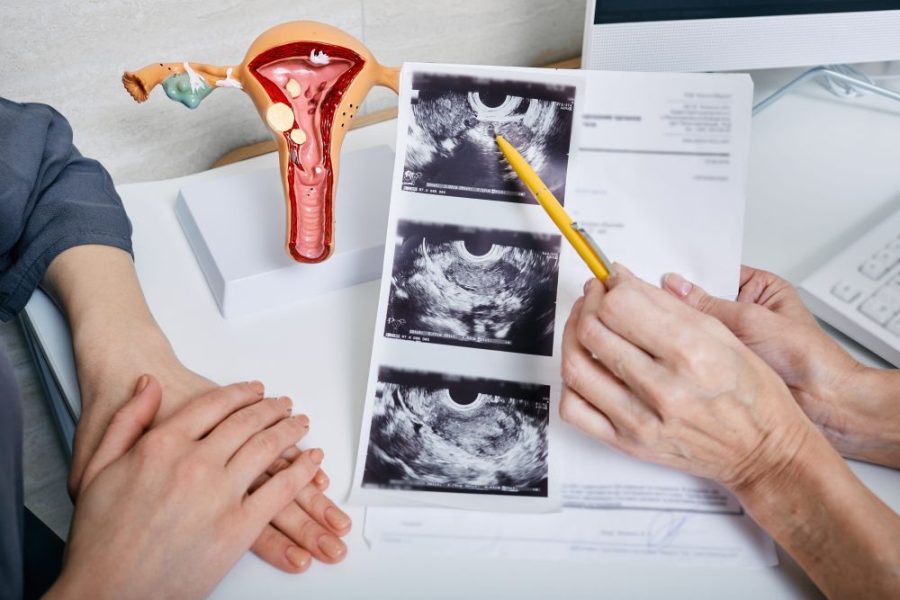
Embryo chromosome testing is a medical tool that screens for embryos for abnormalities before transfer to the uterus. This helps increase the chances of pregnancy and reduce the risk of miscarriage caused by chromosomal abnormalities. While unexpected results may cause anxiety, the information obtained helps doctors analyze the cause and adjust the treatment plan for the next cycle to better suit each couple. Therefore, collaborative planning with a doctor, coupled with continued health care, is a crucial approach to increasing the chances of success and boosting confidence for couples in family planning.
For many couples, the journey to becoming parents may not be as smooth as expected, especially when undergoing infertility treatment and facing unsatisfactory results. One of the most worrying situations is when an embryo fails chromosome testing, leading to questions about the true cause, the meaning of the results, and the appropriate treatment plan for the future.
What is embryo chromosome testing? Is it necessary for couples with infertility?
Embryo chromosome testing, or PGT-A, is a screening process to check for normal chromosome counts in embryos developed through in vitro fertilization (IVF/ICSI) before transferring them back into the uterus.
This test plays a crucial role in helping doctors select embryos with normal chromosomes (euploidy), increasing the chances of pregnancy. At the same time, it helps reduce the risk of miscarriage and minimizes the number of unnecessary treatment cycles, allowing couples to achieve their goal of having children more quickly and safely.
How long does embryo chromosome testing take and what are the steps?
Embryo chromosome testing, or Preimplantation Genetic Testing (PGT), is a high-tech laboratory procedure consisting of these key stages:
Culturing Embryos to the Blastocyst Stage:
After fertilization, embryos are monitored in an incubator until they reach the Blastocyst stage on Day 5 or 6. At this stage, the embryo is robust and has enough cells for an accurate analysis.
Biopsy for PGT-A Testing:
Once ready, an embryologist carefully removes a few cells from the Trophectoderm (the part that develops into the placenta). This process does not affect the inner cell mass that will become the baby, ensuring high safety for embryo development.
Cryopreservation via Vitrification:
After the biopsy, embryos are immediately frozen using the Vitrification technique (flash-freezing). This preserves their integrity while awaiting the detailed genetic results from the laboratory.
Laboratory Analysis:
The sampled cells are analyzed using Next Generation Sequencing (NGS). This modern, high-precision screening identifies whether each embryo has the correct number of chromosomes or specific genetic errors.
Waiting Period for Results:
Typically, the reporting process takes about 7–21 days, depending on the laboratory and technology used. Once results are confirmed, the doctor will schedule a follow-up to summarize the findings and plan the uterine lining preparation for the embryo transfer in the next cycle.
What does it mean if an embryo “fails” the chromosome test?
In medical terms, a “failed” result indicates Aneuploidy, or an abnormal number of chromosomes. Humans normally have 23 pairs (46 chromosomes). Missing or having an extra chromosome—even just one—can affect development. The results usually specify the type of abnormality:
Trisomy (Extra Chromosome):
A specific pair has three chromosomes instead of two. A common example is Trisomy 21, which leads to Down Syndrome.
Monosomy (Missing Chromosome):
A pair is missing one chromosome. This abnormality usually causes the embryo to stop growing or fail to implant.
Complex Abnormalities:
Abnormalities across multiple chromosome pairs. This is often a primary cause of first-trimester miscarriages.
Mosaicism:
A condition where an embryo contains a mix of both normal and abnormal cells. This is a delicate situation that requires close consultation with a doctor to assess the risk percentage before deciding on a transfer.
Causes of Abnormal Embryo Chromosomes
While most chromosomal abnormalities occur naturally, several key factors can directly impact the genetic integrity of an embryo:
Age of Both Partners:
As age increases, the risk of “Non-disjunction” (errors in chromosome division) in egg cells rises significantly. Similarly, advanced paternal age can affect the genetic quality of sperm.
Quality of Sperm and Egg:
Even in younger individuals, poor egg quality or high Sperm DNA Fragmentation can lead to chromosomal abnormalities in the resulting embryo.
Errors During Cell Division:
In some cases, even if the egg and sperm appear healthy, random errors can occur during the rapid cell division phase after fertilization, leading to natural genetic abnormalities.
What to do if the results are not as expected?
If an embryo does not meet the criteria, do not lose hope. This data helps your doctor analyze the root cause and refine the strategy for the next cycle to increase the precision of the treatment.
In-depth Analysis with your Physician:
Your doctor will review the specific abnormalities to evaluate the chances of success and plan a better ovarian stimulation protocol for the next round.
Preparation for a New Cycle:
Doctors may suggest lifestyle adjustments or specific supplements to improve egg and sperm quality for 2–3 months—the ideal timeframe for reproductive cells to regenerate and reach peak health.
Adjusting the Stimulation Protocol:
The doctor may modify the medication dosage or formula to better suit the female partner’s physical condition, aiming for higher-quality eggs and a better chance of achieving a Euploid (chromosomally normal) embryo.
Specialized Testing:
If abnormalities persist across multiple cycles, the doctor may recommend a Karyotype test for both partners to check for hidden genetic conditions (such as translocations) to ensure a more targeted and safe treatment plan.

If you or your partner are facing infertility or have questions regarding embryo chromosome test results and need information to guide your treatment plan—such as understanding what IVF entails—Bangkok IVF Clinic (BIC), a specialized obstetrics and fertility center, is ready to serve as your “Fertility Planner.” We help design a path to parenthood that fits perfectly with your life goals.
We prioritize establishing a clear timeline, advising you on which steps to take and when, so you are fully prepared for the day you become parents. BIC Clinic provides proactive family planning solutions, including egg freezing for the future, ICSI, and Preimplantation Genetic Testing (PGT-A). These services provide essential data to support your decision-making at every stage, all under the expert care and clinical judgment of our physicians.
For more information or to schedule a consultation:
- Phone: +(66) 02-933-1584 to 6
- WhatsApp: @Bangkokivfclinic
References
- Genetics, Chromosome Abnormalities. Retrieved February 10, 2026, from https://www.ncbi.nlm.nih.gov/books/NBK557691/
- Chromosomal Analysis of Pre-implantation Embryos: Its Place in Current IVF Practice. Retrieved February 10, 2026, from https://pmc.ncbi.nlm.nih.gov/articles/PMC7758391/
Frequently Asked Questions About Embryo Chromosome Testing (FAQs)
Q: If both partners are young and healthy, is PGT-A testing still necessary?
A: While being younger generally means lower risk, chromosomal abnormalities can occur randomly in anyone. PGT-A testing is an option that provides “screening for added confidence.” It helps reduce the risk of first-trimester miscarriages and speeds up the time to a successful pregnancy by avoiding the transfer of embryos that may have hidden abnormalities.
Q: If no embryos pass the chromosome test for transfer, how long should I rest before starting a new cycle?
A: Generally, doctors recommend resting for about 1–2 menstrual cycles to allow the ovaries and hormone levels to return to their baseline state. This period is a “golden opportunity” to enhance the quality of eggs and sperm through vitamin supplements, adequate rest, and stress reduction in preparation for the next stimulation cycle.
Q: How comprehensive is the PGT-A result in confirming total health?
A: The test focuses on checking whether the number of chromosomes is correct (such as Pair 21, which is linked to Down Syndrome). However, it does not cover single-gene disorders or certain physical/structural birth defects.